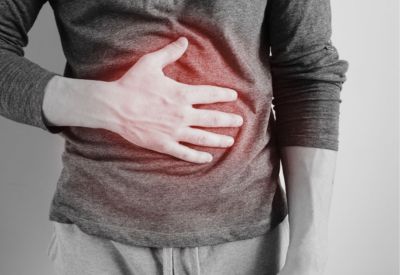
When athletes sustain a direct blow to the abdomen known as blunt abdominal trauma the impact might seem minor at first. Yet internal organ injury, internal bleeding or delayed rupture can carry serious, even life-threatening risks. Awareness, timely evaluation and management are crucial for safe return to play.
Glimpse:
Though rare in sports, blunt abdominal trauma poses substantial risks especially to organs like the liver, spleen or kidneys. Signs can be subtle: pain, nausea, shoulder referred pain or vital-sign changes. Evaluation often involves ultrasound or CT imaging, and many cases are managed non-operatively if stable. But missed injuries or delays can lead to complications or forced long sidelining.
Blunt abdominal trauma in sports, though relatively rare, poses serious risks due to its potential for hidden internal injuries. It typically results from a direct blow to the abdomen such as a collision, fall, or impact from a ball or elbow without skin penetration. While external signs like bruising may be visible, internal organ damage can remain undetected initially, necessitating prompt medical evaluation and vigilance. The spleen is the most commonly injured organ, followed by the liver, kidneys, and occasionally the intestines or pancreas. Even non-contact sports can lead to such trauma through awkward landings or collisions with hard surfaces.
Clinically, athletes may present with a range of symptoms from localized pain to systemic distress. Warning signs include persistent abdominal pain, rigidity, distention, and referred pain like Kehr’s sign (left shoulder pain indicating splenic injury). Additional red flags are bruising around the flanks, low blood pressure, rapid heart rate, and signs of internal bleeding such as blood in urine or stool. Since athletes may underreport symptoms, especially during competition, medical teams must maintain a high index of suspicion when the mechanism of injury is significant
Diagnosis begins with trauma protocols Airway, Breathing, Circulation followed by imaging to assess internal damage. FAST or E-FAST ultrasound is a quick bedside tool to detect free fluid, while contrast-enhanced CT scans are preferred in stable patients to identify organ lacerations or vascular injuries. In unstable cases, diagnostic peritoneal lavage or emergency surgery may be required. Radiologists grade the severity, guiding whether observation or intervention is necessary.
Management is often conservative, involving rest, serial examinations, and imaging. Surgery is reserved for severe cases with active bleeding or organ rupture. Athletes can return to play only after complete recovery, confirmed by normal imaging and lab results. Timely intervention typically leads to favorable outcomes, but delayed diagnosis can result in serious complications like sepsis or permanent organ damage.
“When the abdominal hit seems innocuous, that’s when you must watch most carefully because internal injury may be silently evolving.”
By
HB Team