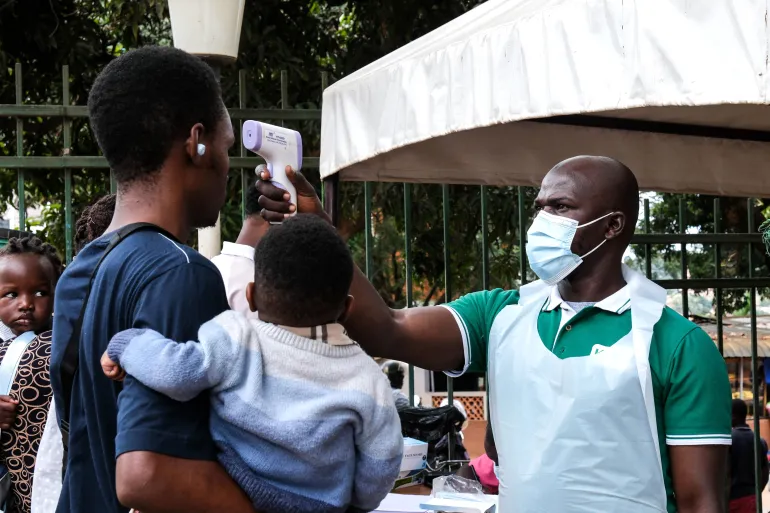
AI bias is emerging as a critical challenge in healthcare, where flawed data and algorithms can lead to unequal treatment, misdiagnosis, and widening health disparities across different patient groups.

Glimpse:
As AI adoption accelerates in healthcare, experts warn that bias in algorithms often caused by unrepresentative data or flawed design can lead to inaccurate diagnoses and unequal care. Studies show that biased AI systems may disproportionately affect minorities, women, and underserved populations, highlighting the urgent need for regulation, transparency, and diverse data.
Artificial intelligence is transforming healthcare by improving diagnostics, treatment planning, and operational efficiency. However, a growing body of research highlights a critical concern AI bias, often described as a “silent risk” that can significantly influence patient outcomes.
AI bias occurs when algorithms produce unfair or inaccurate results due to issues in training data, model design, or implementation. In healthcare, this bias can have serious consequences, as clinical decisions directly impact patient safety and quality of care.
One of the primary causes of bias is imbalanced or unrepresentative data. Many medical datasets historically overrepresent certain populations such as white males while underrepresent minorities. As a result, AI systems trained on such data may perform well for majority groups but poorly for others, leading to disparities in diagnosis and treatment outcomes.
For example, biased algorithms may misdiagnose diseases, underestimate risk levels, or recommend less effective treatments for underrepresented groups. Research shows that such systems can unintentionally reinforce existing social and healthcare inequalities rather than reduce them.
Another challenge lies in algorithm design and historical bias. If past medical decisions or systemic inequalities are embedded in training data, AI systems can replicate and even amplify those biases. This can result in unequal care pathways, where certain populations receive delayed or suboptimal treatment.
The issue is further complicated by a lack of transparency and explainability. Many AI systems operate as “black boxes,” making it difficult for clinicians to understand how decisions are made. This limits trust and makes it harder to identify and correct biased outcomes.
Global organizations, including WHO, have emphasized that without proper governance, AI systems risk exacerbating health inequities rather than improving outcomes. Systems developed without inclusive input or oversight may fail to address the needs of diverse populations.
“Bias in AI algorithms can propagate deeply rooted societal inequalities.”
By
HB Team