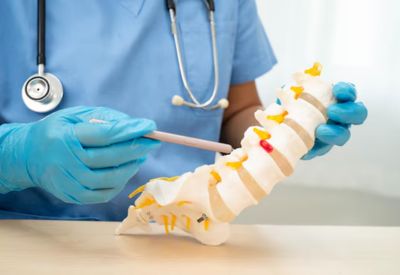
Researchers have developed and validated an AI-driven predictive model that significantly improves treatment decision-making for patients with spinal metastasis. By integrating clinical, imaging, and genomic data, the tool accurately forecasts survival outcomes, risk of spinal cord compression, and response to therapies enabling oncologists to tailor interventions more effectively and avoid overtreatment or undertreatment in this complex patient population.
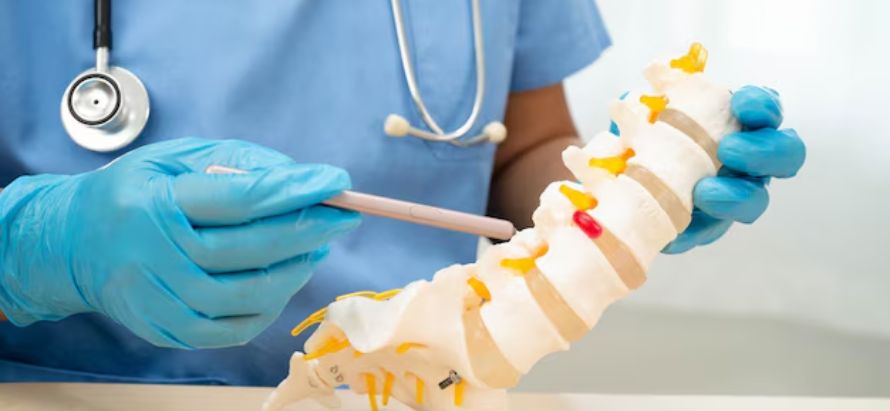
Glimpse:
Published on January 23, 2026, in The Lancet Digital Health, the model was trained on a multi-institutional dataset of over 2,500 patients with spinal metastasis from various primary cancers. It demonstrated superior performance compared to traditional scoring systems (e.g., Tokuhashi, Tomita), correctly predicting 12-month survival with 85–90% accuracy and identifying high-risk patients for urgent intervention. The tool is now being piloted at several major cancer centres and is expected to support shared decision-making, optimise radiotherapy and surgical planning, and improve quality of life for patients facing spinal metastatic disease.
A collaborative research team from leading cancer institutions has introduced a sophisticated AI model that promises to transform how clinicians manage patients with spinal metastasis a condition where cancer spreads to the spine, often causing severe pain, neurological deficits, spinal instability, and cord compression. The tool integrates diverse data streams patient demographics, primary tumour type, performance status, imaging features (MRI/CT), extent of metastatic spread, and molecular/genomic profiles to generate personalised risk predictions and treatment recommendations.
Spinal metastasis affects up to 40% of patients with advanced cancer, particularly those with breast, lung, prostate, and renal primaries. Treatment decisions are complex, balancing symptom relief, preservation of mobility and neurological function, and overall survival prognosis. Existing scoring systems like Tokuhashi, Tomita, and Spinal Instability Neoplastic Score (SINS) have limited predictive accuracy and struggle to incorporate modern therapies (stereotactic radiosurgery, immunotherapy, targeted agents) or patient-specific factors.
The new AI model was trained and validated on a large, multi-centre retrospective cohort exceeding 2,500 patients, with external validation performed on independent datasets. It employs ensemble learning techniques and multimodal fusion to weigh clinical, radiological, and molecular inputs, producing outputs such as:
- Probability of 3-, 6-, and 12-month survival
- Risk of symptomatic spinal cord compression within 6 months
- Likelihood of benefit from surgery, stereotactic vs. conventional radiotherapy, or systemic therapy alone
- Personalised treatment pathway suggestions with confidence intervals
In head-to-head comparisons, the AI model outperformed traditional scores by 15–25% in discrimination (AUC 0.88–0.92 vs. 0.65–0.78) and calibration, reducing the risk of both overtreatment (unnecessary surgery in poor-prognosis patients) and undertreatment (missing opportunities for decompression in salvageable cases).
The research team, including radiation oncologists, neurosurgeons, medical oncologists, and data scientists, has made the model available as a web-based clinical decision support tool for academic and community practices. It is currently in prospective pilot testing at multiple centres to assess real-world impact on decision concordance, patient outcomes, and clinician satisfaction.
“Spinal metastasis is a devastating complication, and decisions about surgery, radiation, or systemic therapy can profoundly affect quality of life. This AI tool gives clinicians an objective, data-driven layer of insight to personalise care helping patients live better and longer with advanced cancer.”
The model has been designed with explainability in mind, providing transparent reasoning for each prediction (e.g., “High risk of cord compression due to >50% canal compromise + rapid progression on recent imaging”). It is compliant with privacy standards and adaptable to different institutional datasets.
As spinal metastasis becomes more common with improved systemic control of primary cancers, tools like this could become standard aids in multidisciplinary tumour boards, supporting more consistent, evidence-based care across diverse healthcare settings.
“Every decision in spinal metastasis care is high-stakes. This AI model doesn’t replace clinical judgment it enhances it, giving doctors a clearer view of what’s likely to happen and what interventions are most likely to help.”
By
HB Team