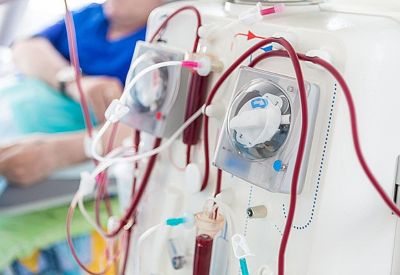
Home-based peritoneal dialysis (PD) could be a game-changer for India’s kidney failure burden but costs, awareness, training, and policy gaps are keeping it from becoming mainstream.
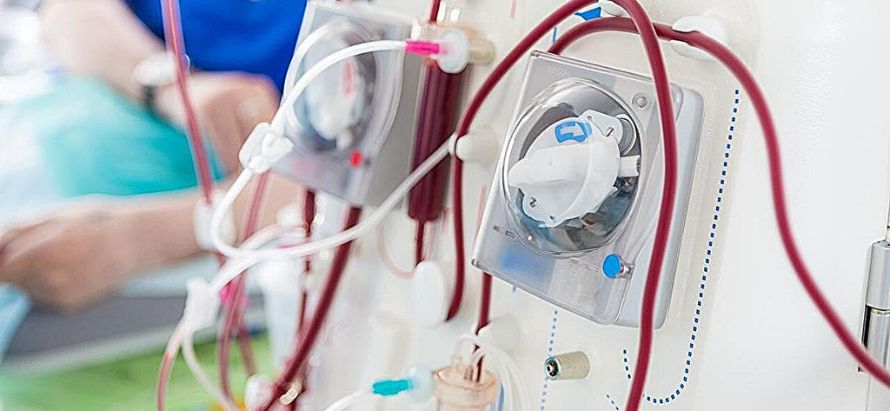
Glimpse:
Peritoneal dialysis offers kidney patients more independence, fewer hospital visits, and lower infrastructure needs than haemodialysis. Yet only a small fraction of Indian end-stage kidney disease patients use PD. Key barriers include high costs for consumables (especially import-dependent supplies), lack of awareness among doctors and patients, limited training, weak reimbursement or inclusion in public health schemes, and regional disparities. States like Kerala, Tamil Nadu, Telangana, Andhra Pradesh, and Chhattisgarh have piloted PD inclusion, but uptake remains low and drop-outs high. Experts are calling for a “PD-first” mindset, better home-based care support, local manufacturing of supplies, and policy reforms to scale PD equitably.
India faces a growing crisis in kidney care: thousands of patients developing end-stage kidney disease each year, limited haemodialysis slots, overburdened hospitals, and huge travel or cost burdens for those in remote or lower-income areas. In this scenario, peritoneal dialysis (PD) a home-based treatment where the patient uses the lining of the abdomen to filter their blood stands out as a powerful, yet under-used, option.
Here’s the rub: despite clear advantages, PD is used by only a tiny minority of patients who need dialysis. According to recent data, only about five percent of all dialysis patients in India are on peritoneal dialysis, even though several states have started including PD in public health programs. Many patients and clinicians still default to haemodialysis (HD), often because HD infrastructure is more visible, hospitals are more equipped, and policies favor HD.
What’s holding PD back?
Cost of supplies & consumables. Many of the fluid bags, catheters, and sterilizing tools are imported or sourced at high cost. This increases out-of-pocket expenses.
Awareness & education gaps. Many kidney patients never hear of PD as a viable option; among nephrologists and primary physicians too, the counseling and training around PD are weaker.
Training and support infrastructure. PD requires caregivers and medical support that patients feel confident about; home hygiene, emergency backup, telephone/remote support, monitoring are all essential but often missing.
Reimbursement & policy limitations. Health insurance or public schemes often cover hospital-based HD more comprehensively. Home PD may not get consistent or sufficient financial support.
Patient factors. Some patients prefer HD because they don’t want to take on the responsibility of home-based therapy; others might be concerned about infection risk, cleanliness, or capacity to manage the supplies daily.
Still, there are bright spots. In places like Kerala, home PD schemes are being rolled out. Some states have started providing PD-related supplies free or subsidised. Expert groups have produced policy and advocacy papers urging changes: a “PD-first” policy, enabling local production of consumables, inclusion of PD in state and national schemes, better training for healthcare workers, telehealth and remote monitoring support for PD users, and more robust patient education.
Scaling up PD could relieve pressure on overcrowded HD units, reduce health inequities in remote areas, and ultimately save costs both for the system and for patients. But for that to happen, India needs conscious shifts in policy, industry, clinical practice, and patient awareness.
“Peritoneal dialysis could rewrite the script for kidney patients far from big cities but only if we make the home option simple, affordable, and supported,”
By
HB Team